On April 26, Peruvian citizen Miriam Grace presented the first symptoms of COVID-19: sore throat, coupled with cough and fever. Warning bells went off when, on May 2, her sister María del Carmen, her nephew Santiago and niece Antonella also showed their first symptoms that went from nausea and vomiting to loss of taste and smell, according to official reports from the Peru Ministry of Health and the interviews that the Center for Investigative Journalism (CPI in Spanish) and Ojo Público conducted with the family.
On May 4, Miriam’s father, Juan Francisco, and María del Carmen fell ill with a recurring cough, and on Saturday, May 9, the virus claimed the only victim in that family, who lived in the same home in the Piura region, north of Peru. Edith, who was the family matriarch, died at home due to a COVID-19 infection, her death certificate confirmed.
In response to this death, personnel from the Peru Ministry of Health went to Edith’s home to perform a rapid antibody test on the five people who had direct contact with her during the last days of her life. Only Miriam Grace, Juan Francisco and María del Carmen tested positive. Santiago and Antonella, who presented the most characteristic symptoms of the virus, were registered as negative before the Peruvian State.

“Those are the most dangerous: false negatives,” said Puerto Rican epidemiologist Andrés Juliá Beltrán, who oversees the COVID-19 situation in Yauco and Lajas, two towns in southern Puerto Rico, about the risk of serological or antibody tests. These tests do not detect the virus itself, but the antibodies that are present in our blood when we become ill with COVID-19, and that can take up to two weeks to show after becoming infected. In other words, a person who is in an early stage of the disease can test negative for antibodies, even if they already have symptoms and are infected.
As in the case of Peru, Juliá Beltrán claimed to have several patients who have yielded false negatives to antibody tests in Puerto Rico. He added that this presents a risk since these people often think they do not have the virus when they test negative, and they infect others.
This was the case of a 50-year-old woman from the town of Ciales, who came in mid-May to Puerto Rico from the U.S. to visit her family. She already had some COVID-19 symptoms, such as fever and cough, and her son had tested positive in the U.S. Three days after flying to the island, an antibody test was done and it was negative. A week later, the symptoms worsened and she was hospitalized. It was not until then that a molecular test was performed, which came back positive. The woman died one day after learning the test result.
A total of at least 17 COVID-19 infections have been confirmed in this town connected to this case. It is the largest chain of contagion that has occurred in Puerto Rico from a traveler, according to epidemiologist Luis Mayol, who leads the epidemiological response in Ciales, a town in the center of the island. As of August 7, this town had registered a total of 73 patients with this new strain of the coronavirus.
Molecular tests do not detect antibodies, but rather the presence of the virus. Although they can also give false results if they are done on the same day that the infection occurs or when the person has been infected for a long time, they have proven to be the most accurate.

Nearly a dozen epidemiologists and health experts interviewed recommend that a person’s contagion always be confirmed by a molecular test, the only test recommended by the World Health Organization (WHO) to confirm that a person has COVID-19. In the U.S., the Food and Drug Administration (FDA) also allows antigen testing that detects virus material for diagnosis. Antibody or serological tests must be complementary to molecular tests as part of the medical evaluation, or for research purposes, such as determining the prevalence of the virus in a community.
Most of the 52 countries in Latin America and the Caribbean have followed WHO’s recommendation and steered their efforts to buying and performing as many molecular tests as possible. But Puerto Rico, Peru and Venezuela followed another road, prioritizing the use of the antibody test to identify COVID-19 in their population, according to an investigation by the CPI, in collaboration with Peruvian media outlet Ojo Público.
In Brazil, the country allows the use of antibody tests for diagnosis, contrary to the recommendations of health experts, if the person has had symptoms for more than seven days when they test positive, according to the Brazilian Ministry of Health’s protocol.
COVID-19 data reported by Ecuador wrongly combines the results of serological and molecular tests in the total number of confirmed cases, when they should only include those obtained by molecular testing.
A mistake in public policy
Since March, several times a day and in different ways, a group of Puerto Rican scientists use as best as they can the 280 characters that Twitter allows them to scrutinize the Puerto Rico government’s response to the pandemic. One of their main complaints has been the misuse of antibody tests and the lack of urgency to increase molecular testing capacity. They have raised their voice not only on social media, but also in letters to Gov. Wanda Vázquez Garced, academic forums and media interviews.
“The [antibody] test doesn’t tell you where the virus is. To control the pandemic, you need to know where the virus is and prevent contagion. You cannot prevent contagion when you’re seeing what happened two weeks ago,” said Mónica Feliú Mójer, doctor in neurobiology and communications & scientific outreach director at Ciencia Puerto Rico, referring to the time it takes for a person to develop antibodies after infection.
Despite this, countries such as Puerto Rico, Peru and Venezuela have bet on serological or antibodies tests, as a method to identify who has the virus. They have served as a diagnostic tool or as a filter to perform a molecular test, against expert recommendations.
Between April and May 2020, antibody tests represented around 50% of the total tests carried out in Puerto Rico, according to figures registered in the Department of Health’s BioPortal, a platform used to centralize information on the epidemic. The agency experiences delays in the reporting of serological tests. In July, it was still adding results of tests done between April and June, according to reports published by the agency.
Meanwhile, in Peru, 73% of the more than 350,000 positive cases reported up to July 20 correspond to antibody tests. “Peru is the country that has done the most diagnoses with rapid tests,” said the WHO representative in that country, Rubén Mayorga, in an interview with Peruvian media this week. To counteract this situation, the Pan American Health Organization donated supplies in mid-July to Peru’s National Institute of Health to carry out 300,000 molecular tests.
In Ecuador, while the government claims that it only uses molecular tests for diagnosis, it includes positive antibody test results in the total number of confirmed COVID-19 cases, according to the government’s daily reports. Of the 91,969 cases reported as of August 7, 10% correspond to antibody tests.
Brazil and Venezuela use both molecular and antibody tests, but neither discloses data on the tests they carry out. The scope of antibody tests in the number of infections they report is unknown.
According to the United Nations Office for the Coordination of Humanitarian Affairs, Venezuelan authorities reported a total of 697,691 COVID-19 tests as of May 21. Of this number, that entity estimates that only 16,577 were molecular tests, or 2%.
The Venezuelan government recently announced that it will “increasingly” change the PCR diagnostic system, but provided no further details.
WHO and Johns Hopkins University report flawed data
The WHO database reflects incorrect figures for Puerto Rico, Peru and Ecuador, which do not meet the health entity’s definition of a confirmed case. The same problem occurs with the Johns Hopkins University’s dashboard, another benchmark in virus surveillance worldwide.
The WHO has been showing as confirmed cases the total number of positive cases (molecular and mixed antibody) reported by Puerto Rico, Peru and Ecuador, rather than just those by molecular testing. It does this despite the fact that the three countries have separate data available on daily molecular and antibody positive tests.
The WHO and Johns Hopkins University did not answer questions about the findings in this story.
On April 6, the government of Peru announced that it began using rapid tests throughout the country. Since then, it has published a breakdown between rapid and molecular tests.
Peruvian President Martín Vizcarra said: “We didn’t want to add the results of rapid tests with molecular tests, which are what we report every day, to avoid creating any type of distortion.”
But there has been distortion. This has led, for example, to a mistake in the positivity rate, an indicator that shows how many positives there are among all the tests that are done. Peru calculates this number using both types of tests combined, rather than the number of molecular tests only, as done around the world.
Peruvians are third in the region in cases per million inhabitants, but only if the results of both tests are combined, as it happens in the WHO and Johns Hopkins University databases. By considering only confirmed cases with molecular testing, more than 10 countries would be above Peru. This doesn’t mean that there are fewer infections in Peru, but rather that there is less certainty and visibility about the situation in real time, several of the experts consulted explained.
“The confirmed case is the one that is positive to COVID-19 tests with the protein polymerase chain test [PCR],” said Dr. Marcos Espinal, director of communicable diseases of the Pan American Health Organization (PAHO), the WHO’s satellite agency in the Americas.
Although it is up to each country to decide how to use the tests it acquires in its battle against the coronavirus, the doctor confirmed that the vast majority of countries in the region follow WHO’s recommendation.
Espinal said that a team at PAHO reviews the data it receives from the different countries in the region. But the WHO continues to report wrong data for Ecuador, Peru and Puerto Rico, despite the fact that since June 10, the island has reported its segregated confirmed cases following the WHO guidelines.
Puerto Rico began using the CDC and the WHO’s definition of a confirmed case two months after the CPI revealed that confirmed cases reported by the government included positive antibody test results, without having a positive molecular test to back it up.

“We are definitely working on many things that we have not done or that we have done wrong,” Health Secretary Lorenzo González said at the time, admitting that the agency had to correct the definitions it uses, including that of confirmed cases.
Now the government of Puerto Rico speaks of confirmed cases only through molecular tests. Those who test positive for antibodies are considered probable cases awaiting confirmation by a PCR test, according to the new protocol.
The Department of Health classifies as “probable cases” only those patients with positive results to serological tests. However, according to the CDC, such a probable case must also include clinical criteria (for example, having symptoms or respiratory problems) or epidemiological evidence.
Dr. Raúl Castellanos, PAHO coordinator in Puerto Rico, declined a request for an interview.
Millions of dollars in antibody tests
In mid-March, when most countries were concentrating their efforts on purchasing molecular tests, Puerto Rico and Peru opted to procure large quantities of antibody tests to detect the virus in the population.
This was done despite the fact that antibody tests were already under fire in places such as Europe due to their low effectiveness and validation problems.
In Puerto Rico, the Department of Health purchased more than 1.3 million antibody tests to detect the disease among the nearly three million residents on the island. Molecular testing took a backseat: the agency only bought 50,000 kits from Quest, which were added to the materials provided by the CDC, which allowed it to carry out 10,000 molecular tests, during the first two months since cases were documented in Puerto Rico.
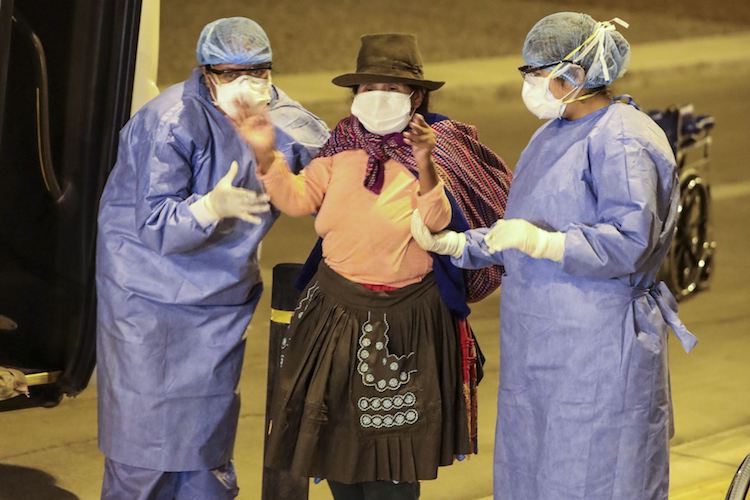
At the same time, in Peru, President Vizcarra announced the purchase of 1.4 million antibody tests and 10,000 molecular tests to diagnose COVID-19. The procurement of antibody tests responded to a “fast track” strategy to detect those infected and stop the spread of the disease, according to the official version.
Peru’s central government has purchased more than 5.2 million antibody tests at a cost of 107.7 million soles, or nearly $30 million. Puerto Rico, which was about to shell out $38 million for 1 million of these tests but canceled the transaction amid irregularities, has allocated more than $9 million for more than 350,000 antibody tests.
The procurement of this type of test on the island came as a recommendation from a task force comprising doctors who advise the government. Its low cost and relative availability compared to molecular tests were factors in this decision, two sources told the CPI.
The transactions were riddled with irregularities. More than a million tests never arrived and were paid at a premium, to people linked to the political party in power. For example: The government of Puerto Rico purchased 200,000 Orient Gene-brand antibody tests at $26 each.
A day later, Peru got the test of the same brand for less than $4.
Also, there were reports of false results due to the low effectiveness of these tests. Three of the four brands the government of Puerto Rico bought were withdrawn from the market because they were not approved by the FDA: Phamatech, Novatest and more recently, Clarity.

In Peru there was also debate about the acquisition of this type of test. The former head of the National Institute of Health, Ernesto Bustamante, criticized the purchase of antibody tests for its low effectiveness and false results due to the time it takes for a person to generate antibodies to COVID-19.
In late March, the Peru Ministry of Health (Minsa, in Spanish) assured that the antibody tests would be complementary to molecular tests and for epidemiological surveillance. However, the medical committee that advises Minsa said something else: antibody tests would be used for diagnosis in symptomatic people after six days from the onset of symptoms.
In mid-April, Peru revised its protocols to establish that antibody tests would be used only for epidemiological surveillance purposes, particularly to identify asymptomatic people.
Antibody tests have a purpose
“If I want to backup my diagnosis and know how long each patient that I have already done molecular tests on has been infected, it works. If I want to know if it’s time to start relaxing [containment] measures, it works. If I want to know what percentage of my population got sick, it works. If I want to know in which region there were more cases or where the virus spread more, it works,” said Thalía García Telléz, a Mexican doctor based in Paris, who specializes in immunology and infectious diseases.
“Its main purpose isn’t to diagnose the patient, but to evaluate the behavior of the pandemic,” said Peruvian epidemiologist Cristián Díaz, responsible for health intelligence work in the Lambayeque region, to the North of Perú, and one of the hardest hit areas by the pandemic in this country.

García Telléz warned that administering antibody tests to the population as if they were diagnostic testing, leads to the absence of real-time information on the status of infection. She added that countries can use this type of test when they begin to lift lockdown measures and health systems are no longer saturated, as a tool that allows them to see the behavior of the virus at the community level.
This is what happens in different Latin American countries, as they begin to explore the reopening of their economies. Serological tests have been a useful tool to learn, for example, the behavior of the virus in communities or social groups through “serological surveys.”
Argentina began conducting antibody tests in Buenos Aires subway stations, while Uruguay does random sampling in rural schools that have begun to open. The Dominican Republic has conducted efforts in some neighborhoods, running antibody tests to identify probable cases of the virus in asymptomatic people.

None of those countries have used antibody tests to confirm COVID-19 cases.
“Molecular tests allow you to identify initial stages of infection and, therefore, allow you to buy time to apply isolation measures. On the other hand, the serological test measures the early or late response of the immune system toward the virus,” said Peruvian epidemiologist Edward Mezones, who is a member of the National Scientific Committee of Peru’s Medical College. “In the clinical sense, which is patient management, the number of days [that a person shows] symptoms defines which test to use,” he concluded.
Molecular tests are the ‘gold standard’ in the Caribbean and other regions
Every island in the Caribbean uses only molecular tests as the “gold standard” to diagnose the disease, but they have faced challenges in processing the tests, since they are all sent to the Caribbean Public Health Agency (CARPHA) in Trinidad & Tobago to be processed.
The island of St. Martin, for example, reported that it used serological tests in a complementary way to determine if the person had immunity to the virus. Others, like the U.S. Virgin Islands, omit antibody test results from their daily reports.
The Epidemiologist of the U.S. territory, Esther Ellis, said the serological tests “only indicate past infections and are not comparable with data from PCR (molecular) tests.”
“We keep the antibody testing aspect separate. Our confirmed cases represent positive results for PCR tests. All tests are carried out in the territory unless a private provider sends them off the island to a commercial laboratory like LabCorp,” she said in a written statement.
Globally, some of the challenges in getting molecular testing include price, processing lead time and a shortage of materials such as swabs and viral transportation required to collect the sample. Only a handful of companies control the supply of molecular tests in the hemisphere: Abbott, Thermo Fisher, Roche, Cepheid, LabCorp and Quest (the latter mostly in the United States and Puerto Rico).
The circumstances among countries are different. Peru, Ecuador and Brazil have faced limitations in obtaining the necessary number of molecular tests, while accruing a higher rate of confirmed cases per million people than Puerto Rico (2,571). Brazilians lead with a rate of 13,505 cases, followed by Ecuador with 4,827 and Peru with 3,737.
In the case of Peru, epidemiologists Cristián Díaz, Edward Mezones and Manuel Loayza agreed that through late July, the government chose to use a greater number of antibody tests because using molecular tests implied logistics, trained personnel and decentralized resources that the country lacks.
In some regions of the country, such as Piura, there is only one molecular biologist to process the molecular tests, so most of them were sent to the capital. This has limited processing capacity.
“Even if we had the kits and tools for a million people, logistically it would have been impossible, because we don’t have the technology for [molecular] analysis in all regions. The rapid test, meanwhile, [requires] a drop of blood that can be taken during field work, it takes 15 minutes. The reasons for using it were quite obvious,” said Díaz, who heads the health intelligence office of the Lambayeque Assistance Network, in northwest Peru.
And while Peru was crippled by the virus, the government of Puerto Rico claimed it was keeping the epidemic under control and did not direct efforts to buy more molecular tests. The excuse was always the same: there is a global shortage.
“Although there are other places that have had similar challenges, they have had the will and creativity to deal with the problem,” said Dr. Feliú Mójer.
Given the lack of resources for molecular tests, Uruguay, for example, turned to the public university to create test kits at the onset of the emergency. The country was able to stop infections through molecular testing.
Journalists who contributed to the collection of data for the maps used in this story are: Freeman Rogers (BVI); Tomer Urwicz and Tatiana Oviedo (Uruguay); Shari Avendaño and Katherine Pennacchio (Venezuela); Isabela Ponce (Ecuador); Gabriel Diez and César Sánchez (Bolivia); Alejandra Thais, Milagros Berríos and Iana Málaga (Perú); Ian Cavazos and Guillermo Flores (Mexico); Monserrat Saavedra and Ignacia Velasco (Chile); Fernando Silva (Honduras); Mariela Mejía and Laura Rodríguez Saba (Dominican Republic); Mary Triny Zea (Panama); Irene Rodríguez and Armando Mayorga (Costa Rica); Carla Miranda (Brazil); Widlore Merancourt (Haití); Elaine Díaz, Darcy Borrero Batista and Yohan Amed Rodríguez Torres (Cuba); Efrén Lemus (El Salvador); Ángel Mazariegos Rivas and Lucía Ixchíu (Guatemala); Julián Navarrete (Nicaragua); Micaela Cattáneo and Juliana Quintana (Paraguay); María Tula and Emiliano Suárez (Argentina).



